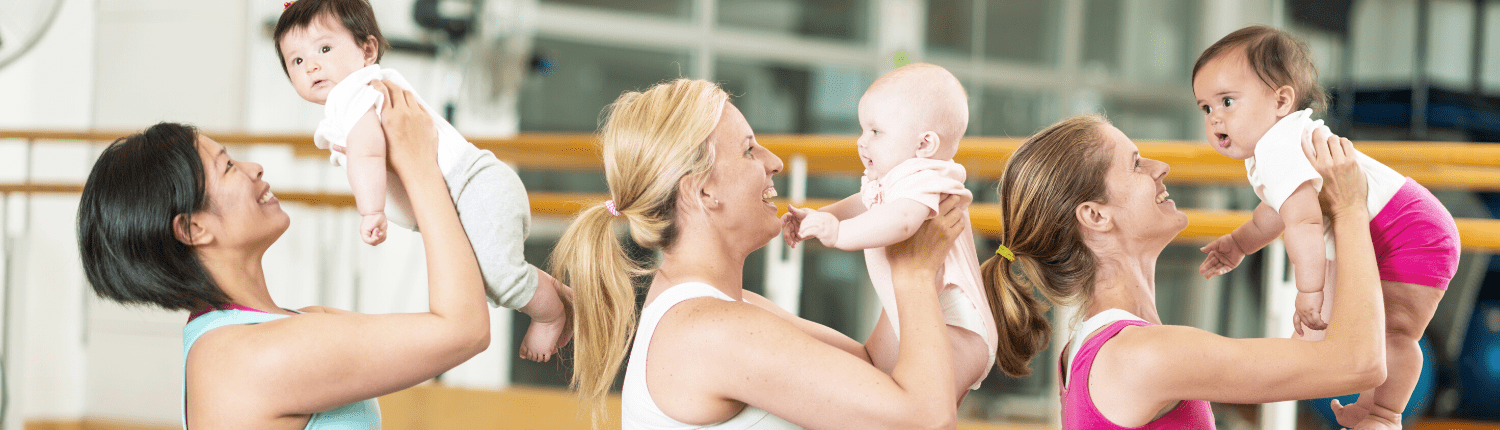A women’s health physiotherapist focuses on treating issues related to obstetrics and gynaecology for women at any time of life – from the teenage years through to the 90’s. Although women’s health physiotherapy is most often associated with treating conditions during and after pregnancy, it’s actually so much more.
Women’s health physiotherapy can help whether you are pregnant, a new mum, recovering from gynaecological and pelvic surgery, experiencing pelvic pain or continence problems. Our specialists are here to help you improve your health, fitness and general wellbeing.
At any time in life
- Overactive bladder and bowel
- Incontinence
- Pelvic pain
- Recovery from pelvic and gynaecological surgery
- Hypertonic pelvic floor
- Pelvic floor weakness
- Endometriosis
- IBS
- Menopause
- Vulvadynia
- Breast cancer management (scar tissue work, shoulder mobility, manual lymphatic drainage)
During Pregnancy
- Pelvic girdle pain
- Carpal tunnel syndrome
- Urinary incontinence
- Back pain (upper, thoracic and lumbar)
- Sciatica
- Rib pain
- Coccyx pain
- Pregnancy massage
We also offer a specialist Pregnancy Health MOT appointment – see more details below
Postnatally
- Urinary incontinence and urgency
- Rectus diastasis (tummy muscle gap)
- Pelvic floor weakness
- Pelvic organ prolapse
- Episiotomy and tears
- C-section recovery
- Musculoskeletal pain (back and neck pain, knee and foot pain, carpal syndrome, de quervain tendonitis)
- Pelvic pain
- Back pain
- Postnatal massage
We also offer The Mummy MOT – see more details below
Pregnancy Health MOT
- A specialist examination provided by our women’s health physiotherapists for pregnant women
- To identify and treat pain or issues you are having during your pregnancy
- Your specialist will provide advice on birthing positions along with exercises and advice specific to you and your pregnancy
- You can book this appointment at any point during your pregnancy
Includes:
-
- A discussion about your medical history, and an in-depth history of your current pregnancy depending on your trimester, any previous pregnancies or deliveries and presenting symptoms and/or challenges.
- Assessment of your pelvis to identify movement issues and/or any pelvic or back pain. We recommend wearing comfortable clothing you can easily move around in. Most of the assessment will be completed in your underwear.
- Discussion and advice around safe birthing positions if you are experiencing any pelvic girdle pain.
- Explanation of pelvic floor exercises to practice throughout and post pregnancy.
- Hands-on treatment to relieve presenting symptoms.
- At the end of the session, we’ll review our findings and go through exercises that are appropriate for you. Your home exercise program will be emailed to you, including videos and instructions, so it’s easy to remember and follow.
Please note we cannot invoice insurance companies for the Pregnancy MOT as this is an additional specialist appointment. Book your MOT online below.
The Mummy MOT
- A specialist postnatal examination for mums after both vaginal and C-section deliveries, no matter how long ago this was
- The aim of the appointment is to assess your pelvic floor, abdominal muscles and check for any prolapses to see how you are recovering after childbirth
- Your specialist physiotherapist will then provide you with treatment and exercises to aid your recovery and return to exercise and fitness
- We recommend booking anytime after 6 weeks postnatal
Includes:
- A discussion about your medical history, and an in-depth history of your pregnancy, delivery, and presenting symptoms and/or challenges.
- Assessment of your breathing, posture, balance, movement, and strength. This includes performing a series of basic exercises. We recommend wearing comfortable clothing you can easily move around in. Most of the assessment will be completed in your underwear.
- Checking your tummy to see how your abdominal muscles/tummy gap is healing (Diastasis Recti) and to check for any hernias. If you have had a C-section, your scar will be checked. If time allows, the session may also include some treatment, such as scar tissue massage.
- An internal pelvic examination to check for any pelvic organ prolapse, assess your pelvic floor function and to ensure you can perform your pelvic floor exercises properly.
- At the end of the session, we’ll review our findings and go through the exercises that are appropriate for you. Your home exercise program will then be emailed to you, including videos and instructions, so it’s easy to remember and follow.
Please note we cannot invoice insurance companies for the Mummy MOT® as this is an additional specialist appointment. Book your MOT online below.
Lactation Physiotherapy
- Specialist physiotherapy treatment for blocked ducts and mastitis due to breastfeeding
Includes:
- Assessment to identify your symptoms – blocked ducts, mastitis or engorgement
- Therapeutic ultrasound treatment to help remove the blockage and treat inflammation with heat and vibration
- Breast massage alongside ultrasound to create movement and release blockage
- Advice, education and referral to a lactation consultant if needed. Please note this appointment does not identify any latch or feeding problems causing your symptoms but it does treat the pain and symptoms. We recommend seeing a lactation consultant to help any feeding or latch problems to stop the symptoms occurring.
Please check with your insurance if they specifically cover this treatment as it is a specialist area or book online below under lactation physio.
Our Women’s Health Physiotherapists
HANNAH SHANKS MCSP Senior Physio
- Bachelor of Science in Physiology with Sports Biomedicine (Hons)
- Masters of Science in Physiotherapy
- Member of the Acupuncture Association of Chartered Physiotherapists
- The Mummy MOT practitioner
- APPI Fully Certified Clinical Pilates with Equipment
- Women’s Health acupuncture
- Pregnancy Health MOT
Hannah graduated with a BSc Hons in Physiology with Sports Biomedicine before completing an MSc in Physiotherapy from Kings College London in 2013. She is a Chartered Physiotherapist with over seven years experience, working in Sports and Orthopaedic medicine in a FIFA Medical Centre of Excellence. Hannah’s underlying philosophy is that “exercise is medicine”, whilst maintaining the traditional hands-on approach. Hannah works holistically to treat the body as a whole in order to resolve pain, and restore movement, strength, and function. This may include a combination of manual therapy, acupuncture, taping, electrotherapy, education, and exercise prescription.
Since having her baby in 2017, Hannah has developed a strong interest in Women’s Health. She is a Mummy MOT® Practitioner and passionate about helping mums recover and achieve their goals from their 6-8 week post natal check and beyond. Having also completed her full APPI Clinical Pilates certification with equipment, Hannah frequently integrates clinical pilates to her rehabilitation programs whereby she is able to help those with musculoskeletal conditions exercise safely and effectively. She is also qualified in Women’s Health Acupuncture which can help conditions such as:
- Over active bladder & bowel
- Incontinence
- Pelvic pain
- Endometriosis
- Pregnancy
- Sickness during pregnancy
- IBS
- Overactive pelvic floor
- Vulvadynia and menopause
In her spare time, Hannah enjoys Yoga, walking her dog, and is a bit of a health and fitness fanatic! She thrives off empowering others, loves being by the sea, and spending time with family and friends.
CARMEN LECH MCSP
- Bachelor of Science in Physiotherapy
- APPI Clinical Pilates – Matwork (Level 1)
- APPI Clinical Pilates – Ante and Postnatal Pilates
- The Mummy MOT Practitioner
Carmen qualified in 2009, with a BSc Physiotherapy (Hons) from St George’s University, London. Following this she went on to work in patient care across several top London teaching hospitals before starting clinical research into the effects of exercise on lung disease.
Driven by her passion for all things Women’s health, Carmen has additional training in Post-natal conditioning, anti and post-natal Pilates (APPI), and is a Mummy MOT® Practitioner. She has a special interest in yoga as medicine, pelvic health, and the menopausal years.
Carmen believes in ageing well and empowering the individual in attaining personal goals and personal health. In her practice she utilises strength and conditioning and breathwork to aid mobility and function.
As a clinician she recognises that pain is multifactorial and the impact that this can have on a person’s life. Her aim is always to improve overall quality of life. She believes in patient-led treatments and the interactive relationship between mental wellbeing and physical rehabilitation.
She uses adjuncts such as myofascial release: scar, remedial, and sports massage to assist in reducing pain and improving functional movement. With a strong belief in the therapeutic benefits of manual therapy she incorporates this skill set, and the importance of education into all treatment sessions. Working hard to support her patients at all times.
Carmen fully supports the individual in achieving personal, relevant goals by providing guidance and support whether it be physical fitness, or a return to activity following injury, illness, or the post-natal period.
She has a good understanding of the importance of lifestyle management and exercise rehabilitation and will incorporate these effectively into your treatment using the full breadth of her expertise.
Whatever your injury or concern, Carmen will provide a thorough assessment and an evidence-based treatment plan, all developed and based on your specific requirements.
When Carmen is not working she’s gardening, raising two small amazing humans, or cycling and exploring the city.
SHAUNA TWEEDIE MCSP
- Lactation support physiotherapy
Shauna is South African and graduated from the University of Cape Town in 2015. She has worked in multiple settings from rural hospitals to private sports practices as well as working with wellness groups within the corporate environment.
She has treated numerous sport’s injuries as well as general injuries linked to our daily activities i.e. neck and back pain, orthopaedic rehabilitation, care of the elderly and blocked ducts/mastitis within women’s health.
Shauna’s skills include hands-on therapy using evidence-based techniques, dry needling, exercise rehabilitation tailored to each individual, as well as massage therapy. She has a keen interest in furthering her knowledge in Pilates and continuously keeping up-to-date with new research.
Shauna recently moved to London with her husband to gain international work and life experience.
She is an active, outdoor person who spends most of her time walking/ running, hiking and traveling.
Shauna has an interest in sports injuries and a passion for helping people overcome their pain and injury to reach their goals.